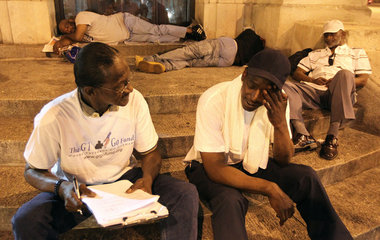
“The more they are suffering, then, the more natural their sufferings appear. Who wants to prevent the fishes in the sea from getting wet? It is terrible that human beings so easily put up with existing conditions, not only with the sufferings of strangers but also with their own. All those who have thought about the bad state of things refuse to appeal to the compassion of one group of people for another. But the compassion of the oppressed for the oppressed is indispensable. It is the world’s one hope.”
~Bertolt Brecht
On my first day of work, as I began to walk the streets of downtown Newark towards my office in the city’s Department of Health, I stared in awe of the Prudential Center, a glittering tower of corporate power, as well as freshly paved roads, police cars on every corner, and manicured public gardens. I began to immediately question how I would imagine my role as a global health activist here. Where was proof of Newark’s highly publicized forms of structural violence, from it being labeled as the fourth poorest city in the nation to one of the most violent spaces on earth? And then, as I began to leave the affluence of downtown Newark and explored the resource-starved wards and neighborhoods of the city, I began to view the similarities between my newfound place of social justice work and ancestral impoverished village of India. On every corner, I noticed an office of a non-profit organization, and realized how Newark had become a republic of NGOs, much like my home of India.
During my first week at work, our Department of Child and Family Well-Being received a phone call from a single mother who desperately pleaded for support to confront her exploitative landlord and investigate his negligence of safe housing codes. She feared raising issues that stripped her three children and her of the right to a healthy environment, as stated in Newark’s Children’s Bill of Rights, a document that gloriously hung on our department walls but its tangible effects experienced sparingly by the community. The lead paint that adorned her apartment walls threatened her children’s cognitive skills, and the dirty water that poured from her taps plagued her children with chronic stomach aches. I began to understand that the structural inequities, such as the lack of clean running water, did not only affect the villages and slums of the developing world, but also devastated the marginalized and forgotten here in the United States.
Before I began working for the City of Newark in August of 2012, I was very anxious working in a country that I mistakenly critiqued as often perpetuating more harm than bringing quality health care to the developing world, where global health policies and research studies were so readily exported to the developing world with no intention to implement the same interventions right here in the U.S. For me, this lack of solidarity between the U.S. and resource-denied countries was exacerbated by the false narrative I comforted myself with, that my efforts were more direly needed in the developing world. I wrongly placed value judgments on the levels of suffering of patients between Newark and the developing world, and I questioned whether I could find the same depth of purpose, passion, and spiritual fulfillment in leaving the “extreme” forms of suffering of orphaned girls of Dehra Dun, India, to the city of Newark.
Yet I soon began to embrace Martin Luther King Jr.’s belief that a threat to injustice anywhere was a threat to justice everywhere. As a Global Health Corps fellow, the abandonment of the notion that one form of suffering was more attention-worthy than another was the only means towards building a culture of solidarity, rather than a model of charity, in the global health movement. Because when we view our suffering as intimately bound to another’s, we liberate ourselves from holding communities to different standards of attentions and care, as we also start to imagine shared solutions to shared challenges between the developed and developing worlds. For example, Dr. Paul Farmer has encouraged the global health community to practice “reverse innovation,” such that Newark can adopt successful best practices, policies, and ideologies from developing countries to its health care system. When the struggles of an HIV-positive incarcerated male in Newark are placed on par with the obstacles of an HIV-positive Nepali refugee in India, maybe we can bring successful models, such as the Indian government’s community health worker program, to the streets of Newark. And then one day, we can rid ourselves of the common narrative that social suffering is “natural” in the developing world and non-existent or scarce in countries like the U.S. I will begin shedding this narrative by stripping my complacency of suffering in a rural village in India, as well as a feeling of shock that Newark possesses higher infant mortality rates than Puerto Rico.
